Ana Carolina Mazzochi

| Anti-Trypanosoma cruzi Potential of New Pyrazole-Imidazoline Derivatives |
| Mazzochi Ana Carolina1, Santos Maurício S.1, Fernandes Pedro H. M.1, Oliveira Edinaldo C. 2, Lara Leonardo S. 2, Orlando Lorraine M. Rocha2, Lanera Sarah C. 2, Souza Thamyris P. 2, Figueiredo Nathalia S. 2, Paes Vitoria Barbosa2 and Pereira Miriam C. de Souza2 1 Laboratório de Síntese de Sistemas Heterocíclicos (LaSSH), Instituto de Física e Química (IFQ), Universidade Federal de Itajubá, Itajubá, 37500-903, Brazil; 2 Laboratório de Ultraestrutura Celular, Instituto Oswaldo Cruz, Fiocruz, Rio de Janeiro, 21040-900, Brazil; |
| Abstract Chagas disease (CD) is a major public health concern. The prevalence of the disease has been documented in 21 Latin America countries, as well as in North America, Europe, Asia and Oceania [1,2]. The protozoan T. cruzi is responsible for CD, and the primary vector of transmission occurs by the bite of the insect vector, popularly known as the kissing bug [3]. Currently, two drugs are available: benznidazole and nifurtimox. These drugs demonstrate high efficacy in the acute phase of the disease, but low activity in the chronic phase. In this study, 13 novel pyrazole-imidazoline derivatives inspired by a previously identified cysteine protease inhibitor were evaluated for their antiparasitic activity. These compounds exhibit low cytotoxicity (CC50 > 100 μM) and efficacy against intracellular amastigotes. Among the 13 derivatives, compound 1k showed high activity (IC50 = 3.3 ± 0.2 μM), selectivity (SI= 73.9) and potency (pCI50= 5.4). The efficacy of this derivative was then assessed in T. cruzi-infected Vero cells (see Figure 1). This derivative was tested in a 3D cardiac microtissue model, which demonstrated a substantial reduction in parasite load. Remarkably, the efficacy of benznidazole was replicated, with comparable outcomes achieved at lower concentrations. The efficacy of benznidazole and the 1k in preventing parasite recrudescence was demonstrated, with the combination of both exhibiting an additive interaction, indicating a potential benefit for in vivo combination therapy. 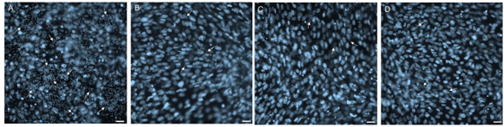 Figure 1. The effect of 1k during a test of washout in infected Vero cells. A. untreated cultures of Vero cells for 4 days. All treated groups were infected for 24 h, treated for 10 days and then monolayers were fixed at 21 days post-infection. B and C. treatment with 1k (28,8 μM and 57,6 μM, respectively) and D. treatment with benznidazole (100 μM). The arrows indicate intracellular parasites. |
| References [1] GOLDENBERG, S.; ZINGALES, B.; COLLI, W. Basic research on chagas disease: Fifty years of successful initiative. Acta Tropica 2025, 265, 1-8. https://doi.org/10.1016/j.actatropica.2025.107598 [2] SOUSA, A. S.; VERMEIJ, D.; RAMOS JR, A. N.; LUQUETTI, A. O. Chagas disease. Lancet 2023, 403, 203-2018. https://doi.org/10.1016/ S0140-6736(23)01787-7 [3] CUCUNUBÁ, Z. M.; GUTIÉRREZ-ROMERO, S. A.; RAMÍREZ, J.; VELÁSQUEZ-ORTIZ, N.; CECCARELLI, S.; PARRA-HENAO, G.; HENAO-MARTÍNEZ, A. F.; RABINOVICH, J.; BASÁÑEZ, M.; NOUVELLET, P.; ABAD-FRANCH, F. The epidemiology of Chagas disease in the Americas. The Lancet Regional Health- Americas 2024, 37, 1-20. https://doi.org/10. 1016/j.lana.2024. 100881 |